What is Atrial Fibrillation?
Source: https://www.cdc.gov/
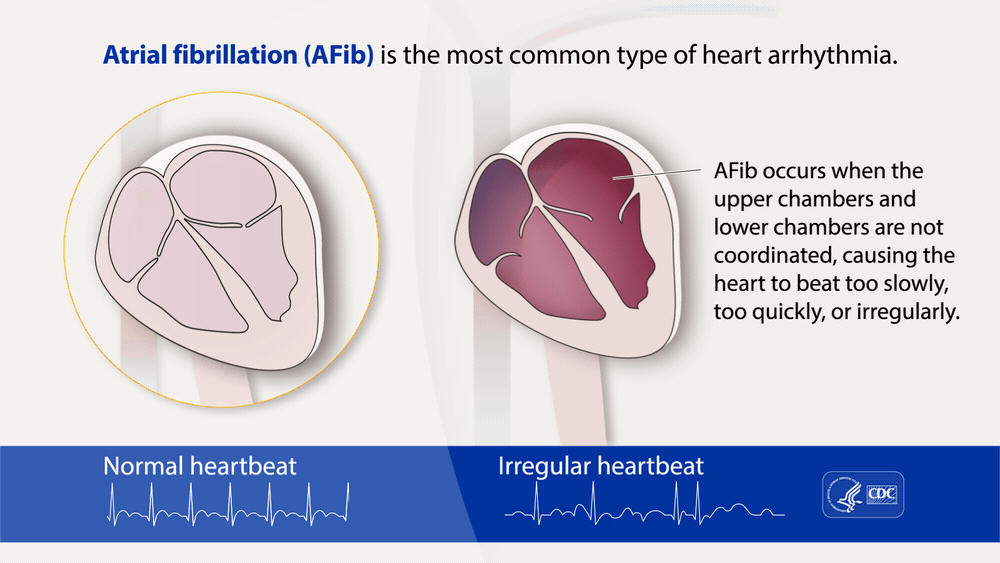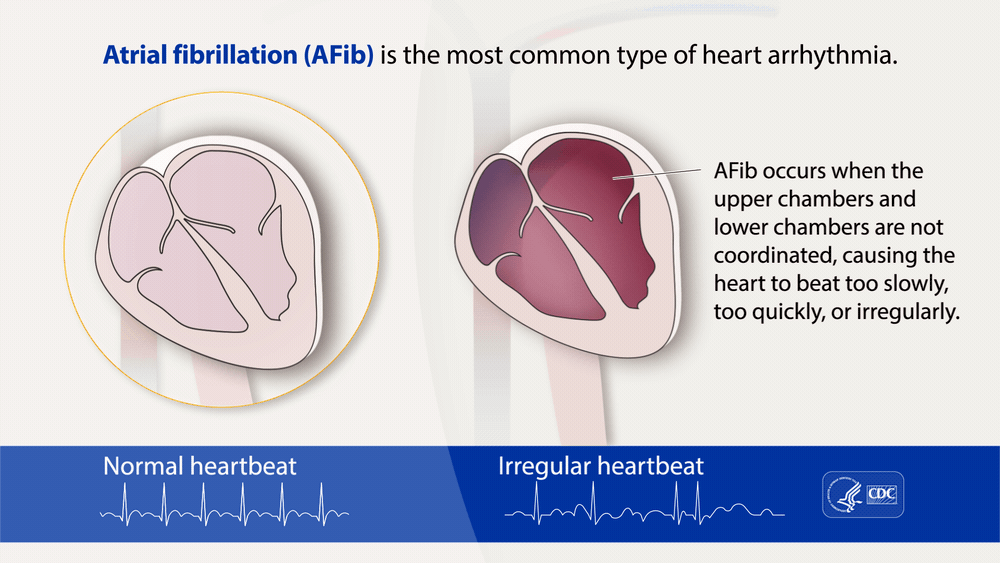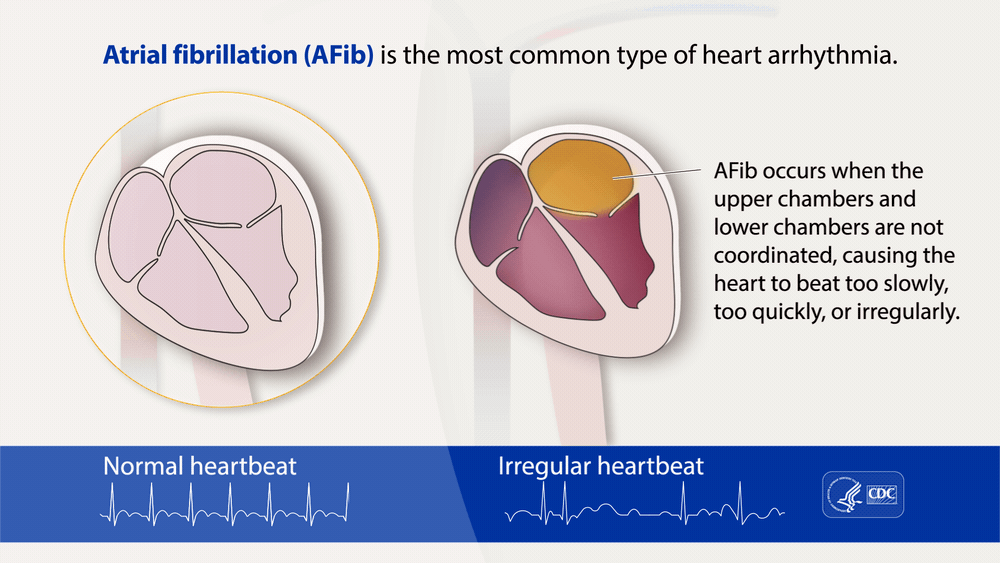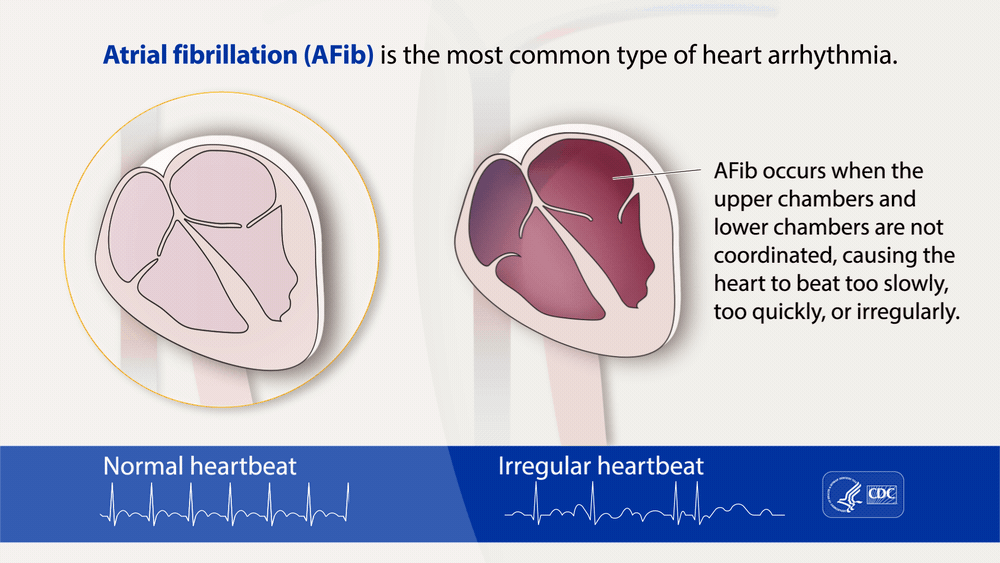
 Atrial fibrillation, often called AFib or AF, is the most common type of treated heart arrhythmia.
An arrhythmia is when the heart beats too slowly, too fast, or in an irregular way.
When a person has AFib, the normal beating in the upper chambers of the heart (the two atria) is
irregular, and blood doesn't flow as well as it should from the atria to the lower chambers of the
heart (the two ventricles). AFib may happen in brief episodes, or it may be a permanent
condition.
Atrial fibrillation, often called AFib or AF, is the most common type of treated heart arrhythmia.
An arrhythmia is when the heart beats too slowly, too fast, or in an irregular way.
When a person has AFib, the normal beating in the upper chambers of the heart (the two atria) is
irregular, and blood doesn't flow as well as it should from the atria to the lower chambers of the
heart (the two ventricles). AFib may happen in brief episodes, or it may be a permanent
condition.
Facts About AFib
- It is estimated that 12.1 million people in the United States will have AFib in 2030.1,2
- In 2018, AFib was mentioned on 175,326 death certificates and was the underlying cause of death in 25,845 of those deaths.3
- People of European descent are more likely to have AFib than African Americans.
- Because the number of AFib cases increases with age and women generally live longer than men, more women than men experience AFib.
What are the symptoms of AFib?
Some people who have AFib don't know they have it and don't have any symptoms. Others may experience one or more of the following symptoms:
High Blood Pressure

Hypertension is the term used to describe high blood pressure. Although African Americans are 40% more likely to have high blood pressure, they are 10% less likely than their non-Hispanic white counterparts to have their blood pressure under control.
Read More facts about Hypertension and how to control or reduce its' effects ...
What are the risk factors for AFib?
The risk for AFib increases with age. High blood pressure, the risk for which also increases with advancing age, accounts for about 1 in 5 cases of AFib.4
Risk factors for AFib include4,5
- Advancing age
- High blood pressure
- Obesity
- European ancestry
- Diabetes
- Heart failure
- Ischemic heart disease
- Hyperthyroidism
- Chronic kidney disease
- Moderate to heavy alcohol use
- Smoking
- Enlargement of the chambers on the left side of the heart
How is AFib related to stroke?
AFib increases a person's risk for stroke. When standard stroke risk factors were accounted for, AFib was associated with a four- to fivefold increased risk of ischemic stroke.6 AFib causes about 1 in 7 strokes.7
Strokes caused by complications from AFib tend to be more severe than strokes with other underlying causes. Strokes happen when blood flow to the brain is blocked by a blood clot or by fatty deposits called plaque in the blood vessel lining.
How is AFib treated?
Treatment for AFib can include
- Medicines to control the heart's rhythm and rate
- Blood-thinning medicine to prevent blood clots from forming and reduce stroke risk
- Surgery
- Medicine and healthy lifestyle changes to manage AFib risk factors
What are the consequences of AFib?
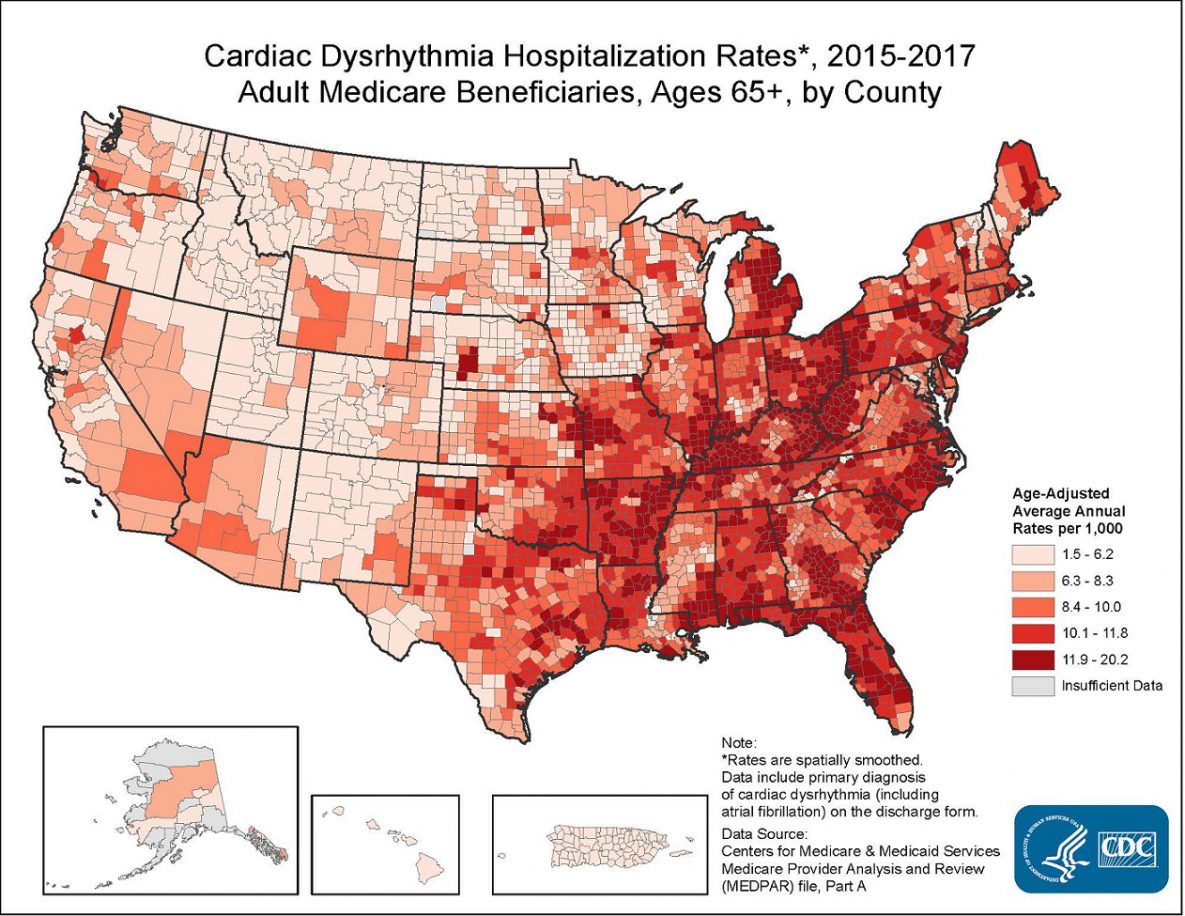
More than 454,000 hospitalizations with AFib as the primary diagnosis happen each year in the United States.4 The condition contributes to about 158,000 deaths each year.3 The death rate from AFib as the primary or a contributing cause of death has been rising for more than two decades.7
More Information
- Million Hearts®
Million Hearts® 2022 is a national initiative to prevent 1 million heart attacks and strokes within 5 years. It focuses on implementing a small set of evidence-based priorities and targets that can improve cardiovascular health for all - Paul Coverdell National Acute Stroke Program
The Paul Coverdell National Acute Stroke Program (Coverdell Program) funds state health departments to collect, measure, and track data to improve the quality of care for stroke patients. - State, Local, and Tribal Heart Disease and Stroke Programs
CDC's Division for Heart Disease and Stroke Prevention (DHDSP) supports state, local, and tribal efforts to prevent, manage, and reduce the risk factors associated with heart disease and stroke. - WISEWOMAN
The WISEWOMAN (Well-Integrated Screening and Evaluation for WOMen Across the Nation) program was created to help women understand and reduce their risk for heart disease and stroke by providing services to promote lasting heart-healthy lifestyles.
Videos and Test Your Knowledge Section
Heart Health I Primary Care with Dr. Lonnie Joe
According to the American Heart Association, nearly 48% of Black women and 44% of Black men have some form of cardiovascular disease.Dr. Kim Williams, Chief of the Division of Cardiology at Rush University in Chicago joins Dr. Lonnie Joe to discuss the key factors contributing to these alarming rates.
OurHealth Media Network
Video 1: Dr. Keith Ferdinand on Atrial Fibrillation Among Blacks and African Americans
Questions for audience before they can move on to next video:
- Data shows that African Americans appear to have less instances of AFib than whites. True/False
- Heart disease is the leading cause of death in the United States. True/False
Video 1a:Keith Ferdinand, MD Discusses Cardiovascular Health
Questions for audience before they can move on to next video:
- There are no health disparities that exist in cardiovascular health. True/False
Video 2:An Overview of Atrial Fibrillation
Questions for audience before they can move on to next video:
- Does AFib causes the heart to raise and beat irregularly? Yes/No
- An Electrocardiogram (EKG) is not used to detect Afib. True/False
Video 3: Complete Guide To Atrial Fibrillation: Causes, Symptoms and Treatments
- The most common symptom of AFib is fatigue. True/False
- Medications used to manage the symptoms of AFib are called antiarrhythmics. True/False
Video 4: Health Disparities Facing Black Communities
The Importance of Exercise and Nutrition in AFib Management
Source: Lifestyle Changes to Manage AFib Better

Develop a better diet
More than almost any other factor, what you eat can affect how you feel. Experts such as the American Heart Association (AHA) suggest that people with AFib adopt a diet low in sodium and fat.
A diet designed for people with heart disease can be helpful for people with AFib. Focus on eating a variety of fresh fruits and vegetables. Flavor your food with fresh herbs or vinegars instead of salt. Use lean cuts of meat, and aim to eat fish two to three times per week.
Keep an eye on K
Food can also impact how successful an AFib treatment is. For example, people who use warfarin (Coumadin) to reduce their risk for blood clots must be aware of their vitamin K intake. Vitamin K is a nutrient found in green leafy vegetables, broccoli, and fish. It plays a role in the body's production of clotting factors.
The consumption of vitamin K-rich foods while taking warfarin can cause unsteady clotting levels. This affects your stroke risk. Be sure to talk to your doctor about the significance of vitamin K intake for your treatment.
Non-vitamin K oral anticoagulants (NOACs) are now recommended over warfarin in part because vitamin K doesn't reduce the effects of NOACs like warfarin does. Talk to your doctor about which medications might be right for you.
Quit smoking
If you've been diagnosed with AFib, it's time to quit smoking cigarettes. Nicotine, the addictive chemical in cigarettes, is a stimulant. Stimulants increase your heart rate and can possibly cause an AFib event.
Additionally, quitting is good for your overall health. Smoking is a risk factor for several chronic diseases, including coronary artery disease (CAD) and cancer. Many people trying to quit have success with over-the-counter smoking cessation patches and gums.
If those aren't successful, talk with your doctor about other medications or therapies. The sooner you're able to stop smoking, the better.
Limit alcohol intake
A glass of wine may help you relax after a long day, but it could cause serious problems for your heart if you have AFib. Studies show that alcohol can trigger an AFib episode. Heavy drinkers and people who binge drink are more likely to experience an AFib episode.
But it's not just large amounts of alcohol that can put you at risk. A Canadian study found that moderate drinking could cause an AFib episode. For men, this would mean having 1 to 21 drinks in a week. For women, it would mean 1 to 14 drinks in a week.
Kick the coffee
Caffeine is a stimulant found in many foods and drinks including coffee, soda, and chocolate. For people with AFib, caffeine may pose a threat since stimulants can increase your heart rate. AFib is sensitive to changes in heart rate, so something that changes your natural rhythm could cause an AFib episode.
But this doesn't mean you have to cut caffeine completely. Drinking too much caffeine could trigger AFib, but a cup of coffee is likely fine for most people. Talk with your doctor about your risks.
Get moving
Exercise is important for both your overall health and the health of your heart. Regular physical activity can prevent a number of conditions and diseases that complicate AFib,
including obesity, diabetes, heart disease, and possibly cancer.
Exercise is good for your mind, too. For some people, dealing with AFib can cause great anxiety and fear. Exercise can help naturally improve your mood and prevent emotional issues.
Take a break
Rest and relaxation are beneficial to your body and your mind. Stress and anxiety can cause dramatic physical and chemical changes, especially to your heart. Proper relaxation can help heal the damage.
If you make time on your calendar for business meetings and appointments, you need to make time for fun too. Give yourself a better work-life balance, and your heart will thank you for it.
Early Detection & Symptom Management
Source: https://www.mayoclinic.org/diseases-conditions/atrial-fibrillation/diagnosis-treatment/drc-20350630To diagnose atrial fibrillation, your doctor may review your signs and symptoms, review your medical history, and conduct a physical examination. Your doctor may order several tests to diagnose your condition, including:
- Electrocardiogram (ECG). An ECG uses small sensors (electrodes) attached to your chest and arms to sense and record electrical signals as they travel through your heart. This test is a primary tool for diagnosing atrial fibrillation.
- Holter monitor. This portable ECG device is carried in your pocket or worn on a belt or shoulder strap. It records your heart's activity for 24 hours or longer, which provides your doctor with a prolonged look at your heart rhythms.
- Event recorder. This portable ECG device is intended to monitor your heart activity over a few weeks to a few months. When you experience symptoms of a fast heart rate, you push a button, and an ECG strip of the preceding few minutes and following few minutes is recorded. This permits your doctor to determine your heart rhythm at the time of your symptoms.
- Echocardiogram. This test uses sound waves to create moving pictures of your heart. Usually, a wandlike device (transducer) is held on your chest. Sometimes, a flexible tube with the transducer is guided down your throat through to your esophagus. Your doctor may use an echocardiogram to diagnose structural heart disease or blood clots in the heart.
- Blood tests. These help your doctor rule out thyroid problems or other substances in your blood that may lead to atrial fibrillation.
- Stress test. Also called exercise testing, stress testing involves running tests on your heart while you're exercising.
- Chest X-ray. X-ray images help your doctor see the condition of your lungs and heart. Your doctor can also use an X-ray to diagnose conditions other than atrial fibrillation that may explain your signs and symptoms.
Symptom Management
Source: https://www.healthline.com/health/atrial-fibrillation/manage-symptoms#treatmentControlling AFib symptoms
The main goal of controlling your AFib symptoms is to prevent recurrent episodes.
When your heart is stimulated or excited, it can trigger AFib episodes. Monitoring your exercise, stress, caffeine intake, and alcohol use can help prevent AFib episodes. Losing weight can also help improve symptoms of AFib.
There are two main options when it comes to controlling symptoms: Bringing your heart rhythm back to normal and controlling the heart rate. Medications are typically prescribed for both options.
Blood thinners or anticoagulants, such as non-vitamin K oral anticoagulants (NOACs), help prevent strokes caused by the irregular beating of your heart. Beta-blockers, calcium channel blockers, and digoxin (Lanoxin) are used to control the heart rate.
Surgical procedures are another option to return your heart rate to normal. Talk to your doctor about what type surgery is right for you if you have persistent AFib, blood clots, or a history of stroke.
Your doctor may decide to do a radiofrequency ablation or insert a pacemaker if you have a slow heart rate. This device sends electrical impulses to the heart muscle to generate a normal heart rate.
Takeaway
One of the best ways to lessen AFib symptoms is to practice a healthy lifestyle. Eating a healthy diet, exercising, and reducing stress are all ways to control your symptoms and lower your chances of serious complications.
National Black Church Initiative would like your help filling out this survey.
If you do not have a Google/Gmail account you can fill this out in your browser's "InPrivate mode" (Microsoft Edge - Ctrl+Shift+N), "Incognito mode" (Firefox - Ctrl+Shift+N) or "Private window" (Chrome - Ctrl+Shift+P).
References
- Miyasaka Y, Barnes ME, Gersh BJ, et al. Secular trends in incidence of atrial fibrillation in Olmsted County, Minnesota, 1980 to 2000, and implications on the projections for future prevalence. Circulation. 2006;114:199–225.
- Colilla S, Crow A, Petkun W, Singer DE, Simon T, Liu X. Estimates of current and future incidence and prevalence of atrial fibrillation in the U.S. adult population. Am J Cardiol. 2013;112:1142–1147. doi: 10.1016/j.amjcard.2013.05.063.
- Centers for Disease Control and Prevention, National Center for Health Statistics. Underlying Cause of Death, 1999–2018. Accessed March 12, 2020.
- Benjamin EJ, Muntner P, Alonso A, Bittencourt MS, Callaway CW, Carson AP, et al. Heart disease and stroke statistics—2019 update: a report from the American Heart Association. Circulation. 2019;139(10):e56–528.
- Benjamin E, Levy D, Vaziri SM. Independent risk facors for atrial fibrillation in a population based cohort. JAMA. 1994;271(11):840-844.
- Wolf PA, Abbott RD, Kannel WB. Atrial fibrillation as an independent risk factor for stroke: the Framingham Study. Stroke. 1991;22(8):983–8.
- Heart Rhythm Society. (2019). Complications from Atrial Fibrillation. Accessed May 9, 2019.
- Centers for Disease Control and Prevention, National Center for Health Statistics. Multiple Cause of Death 1999-2017 on CDC WONDER Online Database, released December 2018. Data are from the Multiple Cause of Death Files, 1999-2017, as compiled from data provided by the 57 vital statistics jurisdictions through the Vital Statistics Cooperative Program. Accessed at http://wonder.cdc.gov/mcd-icd10.html October 4, 2019
